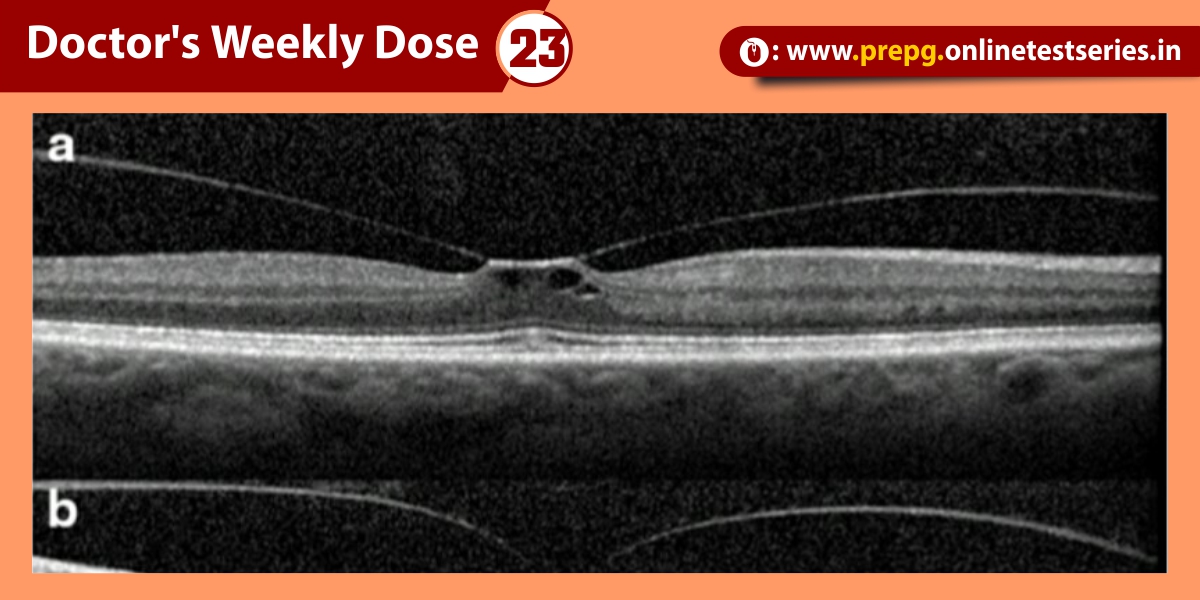
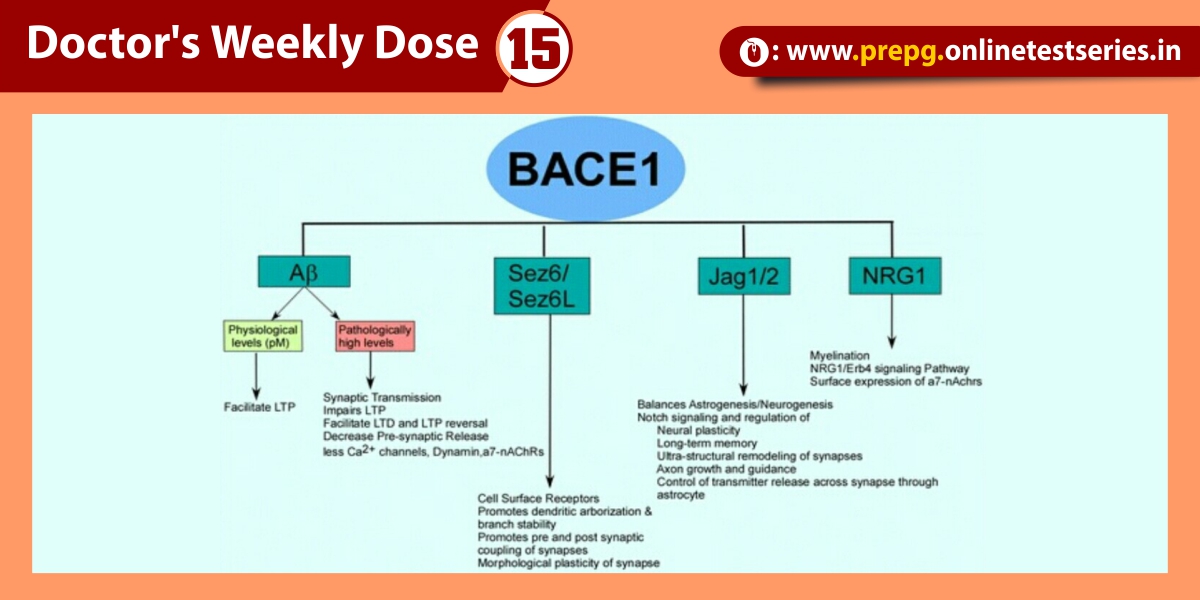
Fuchs endothelial dystrophy (FED) is characterized by an asymmetrical, bilateral, slowly progressive edema of the cornea in elderly patients. When inherited, the transmission is autosomal dominant. Corneal endothelium is a monolayer of cells that acts as the major pump to deturgesce the cornea and ensures clarity. The normal attrition rate of endothelial cells is 0.6% per year; the rate is accelerated in Fuchs endothelial dystrophy. The root cause of the condition is a slowly progressive formation of guttate lesions between the corneal endothelium and the Descemet membrane. These wartlike, anvil-shaped or mushroom-shaped excrescences are said to be abnormal elaborations of basement membrane and fibrillar collagen by distressed or dystrophic endothelial cells. As the lesions enlarge, the covering endothelial cells initially become stretched, and they eventually fall off.
Patients with Fuchs’ corneal endothelial dystrophy and cataract can present a unique challenge to the ophthalmologist. While many such patients have a visually significant cataract and Fuchs’ dystrophy and clearly require combined cataract extraction with endothelial transplant, there are situations where one may proceed with either cataract surgery or Descemet’s stripping automated endothelial keratoplasty (DSAEK) surgery alone.
Decision-making: Cataract extraction alone or combined DSAEK surgery? Several factors must be considered when evaluating a patient with both cataract and Fuchs’ dystrophy. A primary consideration for such patients is the severity and degree of each disease process present. If a patient has significant guttae on exam, documented increasing pachymetry or significant asymmetry on pachymetry, or any evidence of epithelial edema, proceeding with combined cataract extraction and endothelial transplant is recommended.
In addition, if patients report a history of morning blurry vision that clears over the day, consistent with microcystic edema from Fuchs’ dystrophy, despite a mild appearance on exam, strong consideration should be given to proceeding with a combined surgery.
Another key consideration is the patient’s visual demand. Recommendations may differ for the 55-year-old requiring a high degree of visual acuity for many years and the 90-year-old who would like to regain some reading vision. Similarly, one must consider a patient’s ability to provide necessary post-op care for a transplant for an extended period of time compared to post-op cataract care. For patients with visually significant cataracts but with mild guttae and minimal stromal corneal edema on exam, it’s reasonable to proceed with cataract surgery alone, with special attention given to surgical technique as described below so as to minimize traumatic injury to the already diseased corneal endothelium.
Surgical technique Viscoelastic selection: Protection of the corneal endothelium is of paramount importance in patients with mild Fuchs’ dystrophy undergoing cataract surgery. One important way to minimize endothelial trauma is to use a dispersive viscoelastic (e.g., Viscoat, Alcon, Fort Worth, Texas, or Healon D, Abbott Medical Optics, Santa Ana, Calif.) during phacoemulsification. With shorter side chains and lower viscosity, such viscoelastics easily disperse throughout the anterior chamber after injection, providing a true protective coating to the corneal endothelium that lasts longer than cohesive viscoelastics during the operative procedure.
This protective coating serves as a mechanical barrier to excessive ultrasound energy and trauma during phacoemulsification that may otherwise harm the corneal endothelium. Special attention should also be given to removing dispersive viscoelastics from the anterior chamber after phacoemulsification. For the same reasons that they provide a protective coating to the endothelium, these viscoelastics tend to adhere to the endothelium, and if thorough aspiration and irrigation of the anterior chamber is not performed, the patient may be at increased risk of a post-op rise in IOP related to retained viscoelastic obstructing aqueous outflow.
Phaco technique and technology: Specific phacoemulsification techniques may also play a role in the amount of energy produced and resultant trauma to the corneal endothelium. In general, it is recommended that using a phaco-chop technique rather than a divide and conquer technique. This technique allows for less phaco power and phaco time necessary for cataract extraction. Wong et al performed a prospective, randomized study comparing phaco time and phaco power between the two techniques and found similar results. In addition, using advanced phacoemulsification technologies (i.e., torsional or transversal ultrasound), which offer the benefits of increased efficiency in lens removal, greatly reduced repulsion of lens material from the tip, decreased turbulence in the anterior chamber, enhanced followability of lens material, and less risk of thermal corneal wound burns is recommended.
Post-op considerations : A patient with mild Fuchs’ corneal dystrophy who has undergone cataract surgery alone should be followed carefully in the post-op period to ensure clearing of any surgery-related corneal edema. These patients benefit from more frequent steroid use or use of a more potent steroid (i.e., difluprednate 0.05%). In addition, these patients are occasionally given topical hyperosmotic agents (e.g., sodium chloride hypertonicity ophthalmic solution 5% and ointment) in the early post-op period to expedite and ensure deturgescence of the cornea.
Conclusions In summary, while DSAEK surgery provides safe and predictable outcomes for patients with Fuchs’ dystrophy, there are certain clinical scenarios where one may consider cataract surgery alone in a patient with mild Fuchs’ dystrophy.